HEALTH
/ WOMEN, CHILDBIRTH AND HEALTH
Who cries when mothers die?
The probability of an Indian mother dying during childbirth is roughly 10 times that of her Chinese
counterpart. Reducing the Maternal Mortality Ratio (MMR) by three-quarters in 10 years is
now a Millennium Development Goal. Why is MMR in India so high and how far are we from the goal?
Arati Rao
unravels the many challenges to saving mothers' lives.
21 November 2005 -
Lhamu, a mother of twelve, lives in a remote village in Western Tibet. Three of her children died within a month of birth and the four year old strapped to her back looked as small as a one year old. She gave birth all alone, at home, all twelve times. But Lhamu was lucky. She didn't die. One in 33 women dies during childbirth in Tibet. Malnutrition, abject poverty and lack of any health care however basicplagues Lhamu's family, as it does much of Tibet. Tibet vast lonely stretches of dead habit with nary a creature on its harsh plains and no economy to speak of. It can't be as bad here in new economy India, right?
Think again.
One in 48 women in India is at risk of dying during childbirth. The Maternal Mortality Ratio (MMR) in India is a high 407 per 100,000 live births, according to the National Health Policy 2002. Other sources put the MMR at a higher 540 (NHFS and UNICEF data, 2000). Reducing the Maternal Mortality Ratio (MMR) by three-quarters by 2015 is a Millennium Development Goal (MDG) for all countries including India. Achieving this means reducing the MMR to 100 by 2015. Part of the problem is this measurement MMR data is just not there and if it is, it varies widely depending on what method was used to get it.
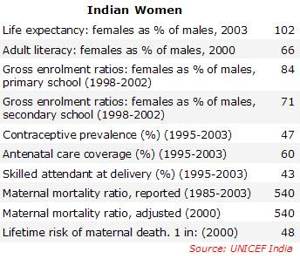
 Studies show MMR among scheduled tribes (652) and scheduled castes (584) is higher than in women of other castes (516, according to one study). It is higher among illiterate women (574) than those having completed middle school (484). The key determinant seems to be access to healthcare. Less-developed villages had a significantly higher MMR (646) than moderately or well-developed villages (501 and 488 deaths, respectively).
Studies show MMR among scheduled tribes (652) and scheduled castes (584) is higher than in women of other castes (516, according to one study). It is higher among illiterate women (574) than those having completed middle school (484). The key determinant seems to be access to healthcare. Less-developed villages had a significantly higher MMR (646) than moderately or well-developed villages (501 and 488 deaths, respectively).
"It is very sad that the numbers are so high even 57 years after independence," avers Dr H Sudarshan who is Vigilance Director (Health) of the anti-corruption body Karnataka Lokayukta. "Not only are the numbers from the Sample Registration System (SRS) high, they are also incomplete. We do not know how many mothers actually died during childbirth and why. Underreporting is rampant and people hide MMR numbers in fear of repercussions. We need state-wise and within states, district-wise data," says Sudarshan who was also Chairman of the Karnataka Health Task Force which made wide-ranging recommendations based on a 2-3 year detailed study conducted in the state. Regardless, the UN MMR numbers for India (540) are several times higher than those for other developing countries like China (56), Brazil (260), Thailand (44), Mexico (83) or even Sri Lanka (92).
Medical reasons
So what exactly leads to such a high MMR? The main reasons for maternal deaths related to pregnancy are anaemia, post-partum bleeding and septic abortions with anaemia being the most rampant. "Antenatal care is most important," declares Sudarshan, "and that is just not being done. This kind of care checks for high risk pregnancies."
Public health advocate Dr Mira Shiva agrees, "Hypertension and the toxemias of pregnancy can only be detected with antenatal care. There is a total neglect of a mother's health in India. [The situation] is disgusting because a big chunk of all this is preventable. The medical establishment is busy with micronutrients but that is not the answer. Giving one iron tablet to a woman during her pregnancy is too late." Shiva is coordinator of the All India Drug Action Network (AIDAN) and one of the founding members of the Peoples Health Movement (PHM). Striking out at a more endemic problem, she says, "The real problem is food. It is all about food, the cost of food and the nutrition content therein. These pregnant women have to fetch the water, make fuel, work the buffaloes, etc., all on the measly amount of food they can afford. How can the nutritive intake be enough? It becomes a negative calorie balance. In short, what is needed goes beyond a medical solution."

Sudarshan echoes Shiva's sentiment, "We need to move from a medical model to a social model. Nutrition for pregnant mothers is very important and the ICDS Anganwadi scheme has clearly not achieved the hoped results." Where antenatal care is good, the results are good as well. Kerala and Tamilnadu have good antenatal care and correspondingly have two of the lowest MMRs in India. In Assam and Bihar where antenatal care is almost zero, the MMRs are among the highest. India has the lowest percentage of antenatal coverage (60%) among countries like China, Brazil, Mexico, Thailand and Sri Lanka which are all in the high 86-95% range.
While antenatal care is paramount in the prevention of pregnancy-related deaths, septic abortions are more insidious. What is worse, the latter tends to go unreported due to the nature and circumstances surrounding it. In many rural areas couples do not use any spacing methods and women conceive within 7 months of having given birth. Dr Leena Joshi of Family Planning Association of India (FPAI) is familiar with this scenario. Her voice drops with concern when she mentions abortion rates in the remote reaches of Maharashtra. "The abortion rate in these areas is just so high. With it comes hidden mortality from septic abortion deaths. Since the PHCs do not have MTP methods, the abortions are performed by quacks. And even if the PHCs or district hospitals have MTP methods, the people opt for local help." Why? "It saves them money. These are very poor people and transport costs and medical costs can be saved by walking to a local quack." As a result there are a high number of abortion-related deaths which do not get reported under maternal mortality. Dr. Joshi laments that everybody only talks about deaths during the childbirth process. "But since there are so many septic abortion cases it all goes unreported."
The problem of unsafe abortion is something that Shiva worries about as well. "Abortion (MTP) being legal in India, no one is turned away. Second trimester abortion is a big reason for rising MMRs." People come late for the abortions and complications ensue. And apparently these are not only driven by spacing problems. "Contraceptives are used only by women and failure of these is common," says Joshi. Of course, abortion of female fetuses is routine and it goes on until the woman conceives a male child. The whole scenario makes one shudder.
But all this seems to be not even half the story.
Take malaria, for example. Orissa has a high incidence and accounted for 28.6% of detected cases of malaria -- 41% of falciparum -- and 62.8% of all material deaths in India (1998). Malaria and pregnancy form a sinister synergistic pair. Falciparum malaria leads to abortion and still births in the gravid woman and can severely compound anaemia. Coincidentally, Orissa has a high incidence of sickle cell anaemia. The combination is lethal. The haemoglobin in pregnant women could drop to 1gm/dL (healthy levels are between 12-16gms/dL). While drugs are available to treat the malaria, the treatment requires a high degree of awareness and care in administration. For example, the common primaquine and tetracycline are absolute no-nos during any stage of pregnancy. But chloroquine and quinine are allowed. "But mistakes occur and are lethal," says Shiva. Acting fast and carefully is paramount and any deaths due to these infections are primarily due to gross neglect or ignorance. Orissa has one of the highest rates of MMR in India at 738.
Another key reason for deaths during pregnancy is post-partum bleeding or haemorrhage. The need for blood in such cases is imperative and access is less than ideal. Both Sudarshan and Shiva worry about the blood bank policy in India. Heavily driven by the HIV/AIDS lobby, they feel that somewhere the important issue of access to blood has been sacrificed for quality and safety since the policy makers are looking at it all from the AIDS perspective. Says Sudarshan,"The policy says you have to keep the blood in an air-conditioned room. But in Coorg, for example, you don't need it. HIV awareness is good, but blood banks need to be demystified and access and availability improved." Shiva adds, "It is imperative in case of complications during pregnancy to have blood available. But no. NACO only sees blood banks from their perspective and only in an emergency are you allowed to take blood from the banks. It is a major concern." When it comes to donation, Shiva points to an endemic problem. The strange connection between men, caring for women, and giving blood. "If the men have to pay a lot of money and go far to get blood for their wives, they just won't. And men will never give blood. They think a 100 drops of blood equals one drop of semen and thus, giving blood is related to potency. And so many times, when women need blood, it is not available."
Organisational reasons
Early diagnosis of high-risk pregnancies and complications and quick referrals are of paramount importance. But is institutionalising deliveries the answer? By requiring 100% institutional deliveries, the World Bank supported vertical program Reproductive Child Health 1 (RCH1) resulted in the abolishing of the dais (Traditional Birth Attendants), and Sudarshan believes, probably increased MMR. Subsequently, following a public uproar, the program was amended to advocate "training" TBAs into Skilled Birth Attendants. "Institutional support will bring down MMR, yes, but what type of institution is important," says Sudarshan. "The so called Primary Health Care units are so dirty that infection will probably increase because of them." "In Bihar, for example," explains Sudarshan, "80% of the deliveries happen at home. In Karnataka it is 70%." Joshi concurs with this high degree of preference. "In the Bhandara area almost 100% prefer home deliveries. And if there are complications, it means there are inevitable delays in getting more sophisticated care."
In India only 43% of deliveries involve a skilled birth attendant compared to between 86% and 99% in Mexico,
China, Sri Lanka, Brazil and Thailand.

Now, if there were a skilled birth attendant (SBA) at the time of each delivery or for antenatal checkups for each pregnancy, he or she can recognize a high-risk pregnancy or a potential complication and refer the mother to a district hospital or closest emergency care unit. The incidence of death from complications would be reduced. Countries like Malaysia have employed this strategy to bring down MMR to less than 100. In India only 43% of deliveries are attended by an SBA compared to between 86% and 99% in Mexico, China, Sri Lanka, Brazil and Thailand.
Sudarshan himself is involved in training tribal girls in the Soliga communities of Karnataka to be auxiliary nurse midwives (ANMs). For a population of 3000, there is a sub-centre and for every 5 or 6 sub-centres, there is a primary health care unit. Sudarshan's team trains the tribal girls in each village so that the few ANMs posted do not have to walk the 20 kms between the 4-5 villages this program covers. Joshi's team in Bhandara also trained 25 local dais or Traditional Birth Attendants (TBAs) to recognize complications and give basic medicines and obstetric care in the villages, one to each village. They also conduct antenatal checkups every month in about 10 villages. But funds for such programs are scant primarily because maternal health is not recognized as a priority issue in India. "The awareness that a pregnant woman should be taken care of is just not there," says Joshi. "If a woman is not delivering, the attitude used to be, let's wait and see, maybe tomorrow morning she will deliver. Now with our training, the dais can recognize complications but the money to shift the patient to a hospital is still not there."
This brings us to the next obstacle. So say the SBA refers to patient to an emergency obstetric care unit (EOC) and let's assume that we have one of those for every few villages. How would the patient reach the EOC? "Transport is a big issue. It is appalling that we do not have EMS (emergency medical services) that is efficient and well staffed," Sudarshan states categorically. He is working on building one for Karnataka with a coordinating body at district level which has jeeps, ambulances, even tractors available for responding to emergency calls. "We have to strengthen the PHC and an EMS is an integral part of that," he says. Bhandara is not so lucky. "Vehicles are available in 50% of the cases. But they are expensive. In the day, people can use buses, but not at nights. There are several rivers in this area and the buses are not allowed to travel over these at night," says Joshi.
Suppose the patient does reach the first referral unit (FRU) with complications that say, require a C-section. Is that a guarantee for a safe delivery? Sadly, no. Few FRUs run 24 hours. Joshi's hospital has 2-3 gynaecologists where the recommended number for the population of that area is 5-6. "All the C-sections and hysterectomies are carried out by these 2-3 gynaecologists. In the PHC in the villages, there is one doctor and 2-3 sisters (nurses), but they are only graduates, not post graduates or MBBS. So they cannot even do a complicated normal delivery, let alone C-sections."
Even in Karnataka, the FRUs are woefully understaffed and in some cases dangerously mismatched. "In one case," says Sudarshan with an ironic smile, "an orthopedist was posted where an obstetrician was required. With bribes, these so-called doctors can get posted to any area they want regardless of what is actually required there." And then there is the big problem of anaesthetists. At the Taluka level there is an acute shortage of them. Anaesthetists are required during complications and surgeries. When Sudarshan's team proposed that nurse obstetricians and other doctors also get trained in anaesthetics, the proposal was shot down by the medical lobby. Human resource management in the health sector seems to be a big issue. Shiva echoed the sentiment saying, "We need trained people in PHCs. And people with the right training. There is no point sending patients who require C-sections to where there is no anaesthetist or ob-gyn."
Government
Now, if we had fully staffed and functioning FRUs, would that bring down the mortality rate? Unfortunately, there is still one more layer that mothers have to contend with.
Shanta lives in a slum in Bangalore. When she was expecting her second child, she had the good fortune of being close to a government hospital where care would be free. Or so she thought. When she reached there, she realized that she had to 'buy' a bed or sleep on the floor. She also had to 'buy' food. So much so that she even had to 'buy' washing services or wear soiled clothes. And when it was time to "push" during delivery, she was just too weak, and the nurses slapped her. Left and right, again and again. They abused and cursed. "Is that the way to treat a patient?" Shanta queries in puzzlement. "My mother's house where I had my first born was better," she declared. Her sister-in-law Prema now laughs as she describes her own run-in with a local PHC outside Mysore. "They wouldn't give me my child until I paid up. Luckily I had saved all year, knowing this would be the case. The nurse was actually someone I grew up with. I thought she would be fair, but no. Everyone wants money." As soon as they got their money, she was sent home - the same day -- with no medicines or follow-up monitoring either for her or her baby.
Corruption is not a new problem. "Even if the most sophisticated PHC is right across the road the ward boy needs to be bribed with Rs 150 to wheel the mother into the operation theatre and another Rs 300 to wheel her to the ward and most cannot afford that," declares a grave Sudarshan. In his opinion this final layer is the most important and toughest one to correct. "Bad governance. The real problem is not technological care but simply what I call the epidemic of corruption in the health services. And this is not just in the public healthcare sector, the private is just as bad," he says. "Doctors in Arunachal Pradesh take their pay checks but never show up. There is rampant corruption in procurement where, in one case, 123 spurious drugs were identified but bribes were taken and they were not reported. Dialysis machines which cost 5 lakhs are bought at 12.5 lakhs. Poor people end up spending huge amounts due to over-prescription of medicines that should be free to them. This is the real problem and no amount of infrastructure improvement will bring down MMR if governance is not improved," warns Sudarshan.
Increasing health spending
"It is great that there will be three times the amount available today for a sector that needs it badly, but one must plug the holes first. No point pouring all that money into a leaky vessel."
-- Dr H Sudarshan

Shiva adds, "The private hospitals are mercenaries too. They perform unwanted C-sections and hysterectomies where none is required simply because there is big money in these procedures." Sudarshan, who sits in the anti-corruption cell of the Karnataka Government has presented strong recommendations to the Karnataka government regarding this issue. He stresses that good accreditation, accountability, good monitoring, and honest reporting are the only things that will actually bring down MMR, given the other necessities are taken care of.
And where will the money for the necessary infrastructure come from? Prime Minister Manmohan Singh has promised that the government spending on public healthcare -- which currently stands at an abysmal 0.9% of GDP (one of the five lowest in the world) -- will be increased to 2-3% of GDP which Sudarshan finds heartening, but tempers his optimism with caution. "It is great that there will be three times the amount available today for a sector that needs it badly, but one must plug the holes first. No point pouring all that money into a leaky vessel," he quips.
So, can it be done? Can MMR be brought down under 100 by 2015?
Sudarshan thinks so, but he will give it not 10, but 15 years. "It all comes down to political will. Sri Lanka, in spite
of the civil war showed tremendous political will in tackling IMR and MMR and setting goals for themselves. Tamilnadu has a Deputy
Commissioner (DC) monitor maternal mortality himself." This has increased the accountability and responsibility of the people in charge and has achieved good results. In Kerala, awareness about maternal health issues is high and the citizens demand more. Literacy plays a key role in keeping the MMR low. Kerala leads the way in successfully reducing MMR and Tamilnadu is close behind. While people like Sudarshan are doing everything to make sure it happens in Karnataka, the awareness and more importantly, recognition of this as an issue is lacking in other parts of India. In Uttar Pradesh, Madhya Pradesh, Bihar, Rajasthan, Assam and Orissa where the MMRs are well above the national average, it will require serious political will and accountability to change status quo.
The Ministry of Health and Family Welfare puts plans in place with the best of intentions (see here), but until governance and administration is addressed, people like Prema will still have no guarantees of care without paying beyond their means to like other pockets. But whether we will make progress will also be determined by when the Ministry recognizes MMR itself one of the key "Health and Population Indicators." Today, they do not. (See here.)
Both Shiva and Sudarshan agree that what India does not require is yet another vertical program to tackle maternal mortality. Verticals tend to be donor driven and cost intensive. MMR is not a disease unto itself. Clearly, high MMR is a symptom of a larger and wider problem in healthcare, namely the overall health of the woman, and should be treated as such and across verticals. Tackling a lot of the broader issues of governance and infrastructure should bring down the MMR. The National Rural Health Mission aims to reach across verticals to integrate services and by appointing an Accredited Social Health Activist (ASHA) at the community level provides decentralized first contact care. Shiva was part of one of the Task Forces of the NRHM and lauds its efforts as broadening the RCH program. But in order that the NRHM succeed, we come back to the need for evaluation methods and strong accountability.
The health of mothers is directly related to a child's health and without due attention to the causes behind high maternal mortality ratios, we are ignoring an important determinant of the health of our nation. In doing so, we may be running the risk of damaging our chances for all-encompassing prosperity.

![]() Studies show MMR among scheduled tribes (652) and scheduled castes (584) is higher than in women of other castes (516, according to one study). It is higher among illiterate women (574) than those having completed middle school (484). The key determinant seems to be access to healthcare. Less-developed villages had a significantly higher MMR (646) than moderately or well-developed villages (501 and 488 deaths, respectively).
Studies show MMR among scheduled tribes (652) and scheduled castes (584) is higher than in women of other castes (516, according to one study). It is higher among illiterate women (574) than those having completed middle school (484). The key determinant seems to be access to healthcare. Less-developed villages had a significantly higher MMR (646) than moderately or well-developed villages (501 and 488 deaths, respectively).
























