Way back in 1946, a very forward looking Health Survey and Development Committee, headed by Joseph Bhore, outlined a universal health care plan. Anticipating that large sections of the population may be unable to pay for health care, the committee recommended that no person should be denied medical care because of an inability to pay for it. It also recommended that health workers be on the public payroll, limiting the need for private practitioners. The committee also laid special emphasis on preventive methods and communicable diseases. Moreover, recognizing urban-rural disparities, it laid out an infrastructure plan for a comprehensive three-tier health care system at the district level in order to provide preventive and curative health care to everyone.
That grand design is now evidently in shambles. Six decades after the recommendations of the Bhore Committee were put forward, the nation's actual delivery of health care is among the worst in the world, and the benchmarks for health care set then are still very far from being achieved. Here is one quick measure of how India is tracking, as of 1998, with respect to specific infrastructural recommendations: while the committee recommended 567 hospital beds for every 100,000 people, the country actually has 70, only a little more than a tenth of the recommended ratio.
The investment required back then to achieve the recommended levels of health care services was under 1% of GDP; implementing the Bhore committee recommendations then could have been the recipe for a robust health care system in India today, with a recurring cost of just 1.33% of GDP, according to one estimate. Instead, implementation of health care plans has become fragmented into narrow vertical 'programs' over nine five-year plans, thus losing the essence of a holistic approach. The social welfare ethos of the committee has long been left in the dust, and instead India has allowed the private sector in health care to take its place. As a result, accessible, quality universal health care today is simply a dream for most citizens. Countless numbers of Indians endure the abysmal and scarce routines that pass for medical care instead.
And as if costs were not gross enough, actual care is fraught with shoddiness and corruption. Giri's father-in-law was in an ICU at a local private hospital, suffering from cancer. The medicines required for his treatment cost many thousands of rupees per dose, and had to be bought only at the hospital pharmacy. Giri had to physically take the medicines to the ICU himself, but he was unsure if they were really being administered to his father-in-law. One day, he marked the medicines with a black dot on the underside of the bottle before depositing them in the ICU. His suspicion was confirmed when he noticed that he was given the very same bottles the next time he went to the hospital pharmacy. But he had no recourse to either recover his money, or prove that the ICU staff never used the medicines.
Rights are not enough
The irony is that on paper, India has committed itself to delivering so much more. The Indian constitution is explicit in noting a 'right to life' (Article 21), and India has acceded to the International Covenant on Economic, Social and Cultural Rights. Article 12 of ICESCR refers to "the right to the highest attainable standard of health," requiring availability, accessibility, acceptability and quality as imperatives in health care in along with universal access to the underlying preconditions of good health. Ravi Duggal, who is the Coordinator of the Centre for Enquiry into health and Allied Themes (CEHAT), Mumbai says, "The Indian parliament has ratified it, and as such, it should become law within the country. But no, we are not honouring it."
Not for want to trying by civil society, though. NGOs around the nation have demanded much higher levels of health services from government, and beyond these efforts, the People's Health movement (PHM) too has been involved. Calling upon the National Human Rights Commission (NHRC) to collaborate with PHM, the body organised regional consultations all across India in 2004. At these events, people brought their grievances and "denial of health care" instances and pleaded their cases. The state governments were invited by the NHRC to defend themselves. "It was like a court, almost a formal process," says Duggal. "In the end, the Jan Swasthya Abhiyan - a compendium of evidence concerning Denial of Right to Healthcare - finally brought the Right to Health Care on the government's agenda, and probably, somewhere, influenced the birth of the National Rural Health Mission," conjectures Duggal.
But Rights and Constitutional amendments without legislation to back them are ineffective, in any case. Unless the declarations of rights are backed by law, they are lost to the larger public. "Right to information is ok where people are aware and have NGOs to facilitate," declares Duggal. Where there is a larger civil society, one can use information to demand rights. But health and education are collective rights, not individual rights; how does one assure these entitlements to the larger population? Only through legislation, says Duggal. The PHM is debating the next steps to make this happen, and is contemplating filing a Public Interest Litigation in the Supreme Court to move the government to bring in legislation to make the right to health care established in law. The National Assembly in January 2007 plans to also collaborate with the state and central governments to monitor the progress of the NRHM.
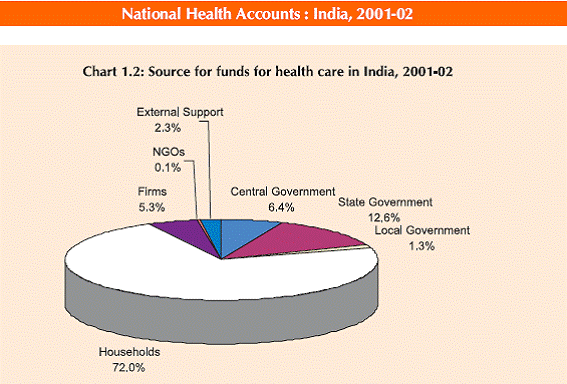
Public expenditure on health care today is a dismal 0.9% of GDP, and growth is gradual. The total expenditure on health in India as a percentage of GDP is almost 5%, with 75% of it being private health expenditure. Of this, 97% comes out-of-pocket. Only countries like Myanmar, Cambodia, Armenia, DR Congo and Azerbaijan, rank higher in terms of private health expenditure as a percentage of total health expenditure. Government expenditure on health as a percentage of total health expenditure in countries like Sri Lanka and Malaysia is almost twice that in India. The Centre/State contributions to expenditure on health as of 2001-2002 National Health Accounts were 6.4% and 12.6%. The ideal scenario, according to a detailed study done by Duggal and CEHAT, is to get government funding of health care up to nothing less than 60% of total health expenditure, with a 35-65 split between the Centre and the State (See Operationalizing Health Care, CEHAT Website). The rest would be borne by the organised sector and other sources.
| Some key Indicators (from the WHOSEA website) | Value (2003) |
| Total expenditure on health as percentage of gross domestic product | 4.8 |
| General government expenditure on health as percentage of total expenditure on health | 24.8 |
| Private expenditure on health as percentage of total expenditure on health | 75.2 |
| General government expenditure on health as percentage of total government expenditure | 3.9 |
| External resources for health as percentage of total expenditure on health | 1.6 |
| Social security expenditure on health as percentage of general government expenditure on health | 4.2 |
| Out-of-pocket expenditure as percentage of private expenditure on health | 97 |
| Private prepaid plans as percentage of private expenditure on health | 0.9 |
| Per capita total expenditure on health at average exchange rate (US$) | 27 |
| Per capita total expenditure on health at international dollar rate | 82 |
| Per capita government expenditure on health at average exchange rate (US$) | 7 |
| Per capita government expenditure on health at international dollar rate | 20 |
But Duggal still gives the government 'brownie points' for arresting the slide in allocation of resources to the health sector. A few states like Maharashtra, Kerala, Karnataka, and Tamilnadu have moved forward on their own, and shown improved resource allocation and intent to make health care efficient. Duggal finds this promising, but cautions against the "World Bank mentality" of measuring efficiency by attaching conditionalities of payment to the delivery of health care. If users have to pay at the time of treatment, the very essence of a 'right' is diminished, he says. "The best health care systems are in any case paid for indirectly through taxes and state funds. The patient should not have to pay for it at the time of delivery. That just won't work."
Indeed, while much is being done via the NRHM and in smaller pockets through various non-governmental efforts, these are fragmented and highly informal efforts, grossly failing to address the imperative of universal health care and a well-functioning public health care system. It seems that until government commitment to health care is formalised and backed up by sufficient investment, and the citizens have recourse to demand information and delivery of health care in a more universal fashion, the "promise of health for all" will remain just that.
























